A doctor in Scotland has been suspended and investigated for failing to follow up on the results of colonoscopies he performed on thousands of patients, some of whom developed cancer and died.
What is a colonoscopy and why is it important?
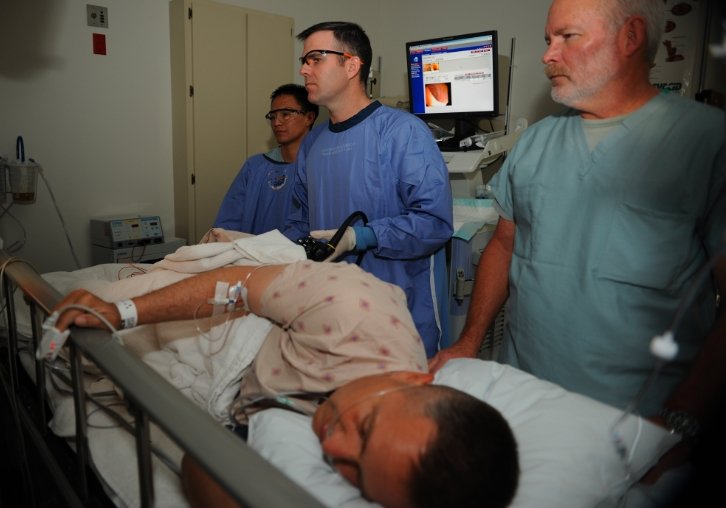
A colonoscopy is a procedure that uses a thin, flexible tube with a camera and a light at the end to examine the inside of the large intestine (colon) and rectum. It can detect polyps, ulcers, inflammation, bleeding, and cancer. It can also remove polyps or take tissue samples for biopsy.
A colonoscopy is recommended for people who have symptoms such as rectal bleeding, abdominal pain, change in bowel habits, or weight loss. It is also used as a screening test for people who are at high risk of developing colorectal cancer, such as those with a family history, inflammatory bowel disease, or certain genetic syndromes. The screening test can help prevent colorectal cancer by finding and removing polyps before they become cancerous.
How did the doctor fail to follow up on the colonoscopies?
The doctor, who has not been named, worked at the NHS Greater Glasgow and Clyde (NHSGGC) health board from 2020 to 2022. He performed colonoscopies on about 2,700 patients, most of whom were part of the Bowel Screening Programme for people aged 50 to 74.
The health board discovered that the doctor did not consistently follow up on the results of the colonoscopies he performed. He did not check if the patients had received their test results, if they needed further investigations or treatments, or if they had any complications or adverse outcomes. He also missed the opportunity to refer some patients to specialists or surgeons who could have treated their conditions.
As a result, some patients did not receive appropriate care and suffered harm. The health board identified six patients who were harmed by the doctor’s negligence, three of whom died. Some of the patients developed malignant tumors that could have been prevented or treated earlier if the doctor had followed up on their colonoscopies.
How did the health board find out about the doctor’s errors?
The health board first became aware of the doctor’s errors in March 2022, when one patient was identified as not receiving appropriate follow-up care after a colonoscopy. The health board conducted a review of the case and concluded that it was an isolated administrative error.
However, in August 2022, another patient was identified with the same issue. The health board then commissioned a more comprehensive review of all the cases managed by the doctor since 2020. The review revealed that there were more patients who were not followed up properly and that there was a pattern of negligence by the doctor.
The health board suspended the doctor in November 2022 and launched a formal disciplinary investigation and a clinical review into his practice. The doctor has since left the employment of NHSGGC.
How did the health board respond to the affected patients and families?
The health board contacted all the patients who were affected by the doctor’s errors and informed them of the outcome of the significant adverse event reviews (SAERs) that were carried out into their cases. The SAERs are independent investigations that examine what went wrong, why it happened, and what can be done to prevent it from happening again.
The health board also offered its sincere apologies and condolences to the patients and families who were harmed by the doctor’s errors. It said that it would ensure that the recommendations and lessons learned from the SAERs would be shared with other health boards and implemented to improve patient safety and quality of care.
The health board also set up a contact number for patients who may have concerns or questions about these issues. Patients can call 0141 451 5435 between 8am and 8pm Monday to Sunday.
How did the authorities and regulators react to the doctor’s errors?
The health board informed the General Medical Council (GMC), which is the regulator of doctors in the UK, of its investigations when it first identified the issues in August 2022. It has continued to update the GMC of its progress and findings.
The GMC said that it was aware of the concerns and was looking into them. It said that it was working closely with NHSGGC and other relevant organisations to ensure that appropriate action was taken to protect patients and uphold standards of medical practice.
The Scottish Government also expressed its concern about the situation and sympathised with all the families affected, especially those who lost a loved one. It said that it noted that NHSGGC took steps to fully investigate what occurred and accepted the recommendations from the SAERs.
What are the implications and challenges of this case?
This case raises serious questions about how colonoscopies are performed, monitored, and followed up in Scotland and across the UK. It also highlights the potential risks and consequences of medical errors and negligence for patients and their families.
According to the latest statistics from NHS Scotland, there were 120,000 colonoscopies performed in Scotland in 2021-22, with a waiting time of 12 weeks for urgent referrals and 18 weeks for routine referrals. The Bowel Screening Programme, which started in 2007, invites eligible people to take a home test kit every two years and refers those with positive results to colonoscopy.
The quality and safety of colonoscopy services are regulated by various standards and guidelines, such as the Scottish Bowel Screening Programme Quality Assurance Standards, the British Society of Gastroenterology (BSG) Quality and Safety Indicators for Endoscopy, and the Joint Advisory Group (JAG) on Gastrointestinal Endoscopy Accreditation Scheme.
However, these standards and guidelines may not be enough to prevent or detect errors or negligence by individual doctors or health boards. There may be gaps or weaknesses in the systems and processes that are supposed to ensure that colonoscopies are performed correctly and followed up appropriately. There may also be challenges in ensuring that doctors are competent, trained, supervised, and audited regularly and effectively.
Therefore, there is a need for more robust and rigorous measures to ensure that colonoscopies are safe and effective for patients and that any errors or negligence are identified and addressed promptly and transparently.


















